Abdominal Aortic Aneurysms
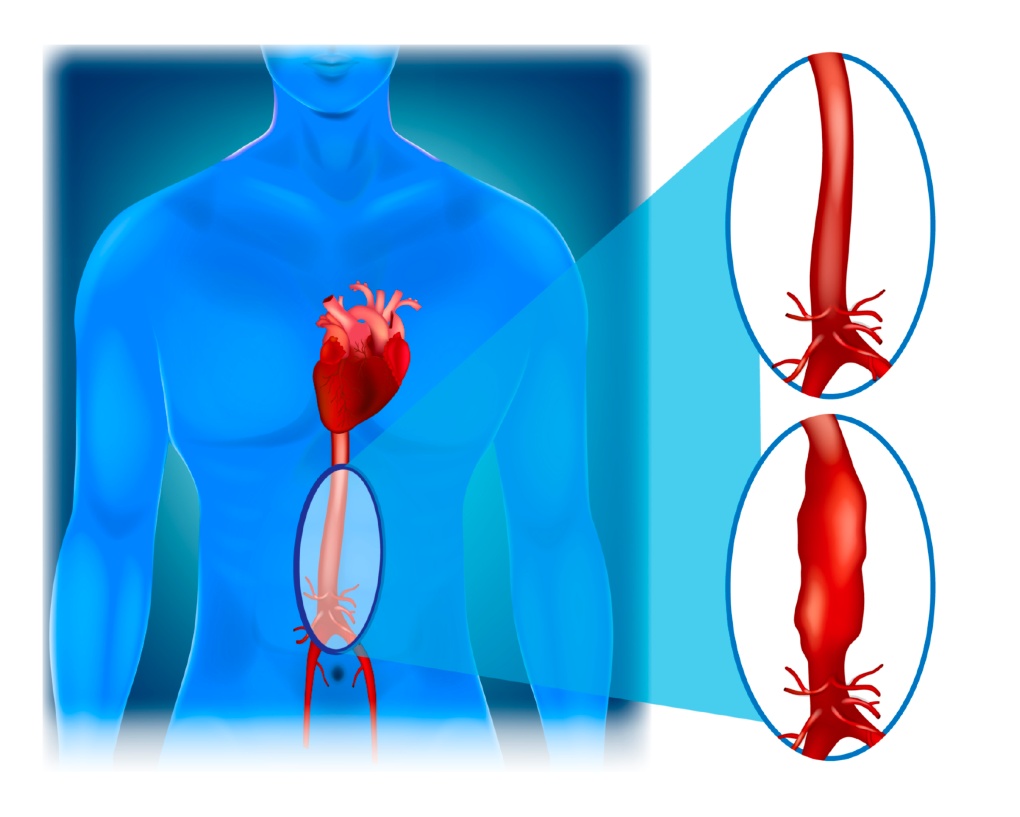
An aneurysm is a localized dilation or bulge in a blood vessel. Abdominal (AAA) and thoracic (TAA) aortic aneurysms occur when the aorta dilates more than 150% of its normal diameter at a particular point.
The larger the bulge becomes, the greater the risk that the aorta will rupture, causing internal hemorrhage. Almost six in 100,000 people will develop an aortic aneurysm. Men are 2 to 4 times more likely to be affected than women, and the average age at the time of diagnosis is 60-70 years of age.
Do I Have an Abdominal Aortic Aneurysm?
Many times physical exam results are normal and patients may experience no apparent symptoms.
However, symptoms may include:
- Back, chest or abdominal pain
- “Pulsing” sensation in the abdomen
- Hoarseness
- Wheezing
- Difficulty swallowing
- Hypotension (low blood pressure)
- Tachycardia (fast heart beat)
- Shock (if the aneurysm ruptures)
Common Risk Factors
- Smoking
- Congenital abnormalities (heredity)
- Infections
- Atherosclerosis
- High blood pressure/hypertension
- High cholesterol
These risk factors can lead to a weakening of the blood vessel wall, allowing an aneurysm to develop. Additional risk factors may exist that can be tested by your physician.
Diagnosis
Fortunately physicians today have many tools at their disposal to help accurately diagnose and treat abdominal and thoracic aneurysms (AAA and TAA.) The first and most important begins with a thorough history and physical.
Tests include:
- Blood work
- Ultrasound
- Contrast-enhanced CT scans
- Magnetic resonance imaging (MRI)
- Contrast angiography
- Chest radiography
- Transesophageal echocardiography
- Ultra Sonography
Treatment options
If we detect AAA or TAA, we typically treat them surgically with a graft, a synthetic portion of blood vessel, replacing the area where the aneurysm was. We may monitor small aneurysms for a period of time to see if they enlarge.
Treatment options include endovascular aneurysm repair and open aneurysm repair.
Schedule a Consultation
Fill out this form or call
239-344-7061 today!
